Category: mHealth
-
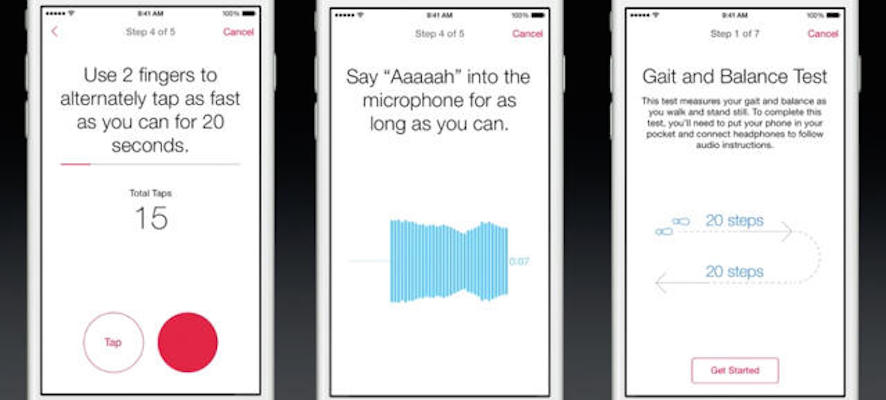
Phone based Parkinson’s research
mPower is a mobile Parkinson’s Disease study, powered by HealthKit. It attempts to understand why people experience different symptoms, and why a person’s symptoms and side effects can vary over time. The process includes surveys and tasks that activate phone sensors. Progression symptoms, including dexterity, balance and gait, are tracked. The goal is to understand variations, improve the…
-
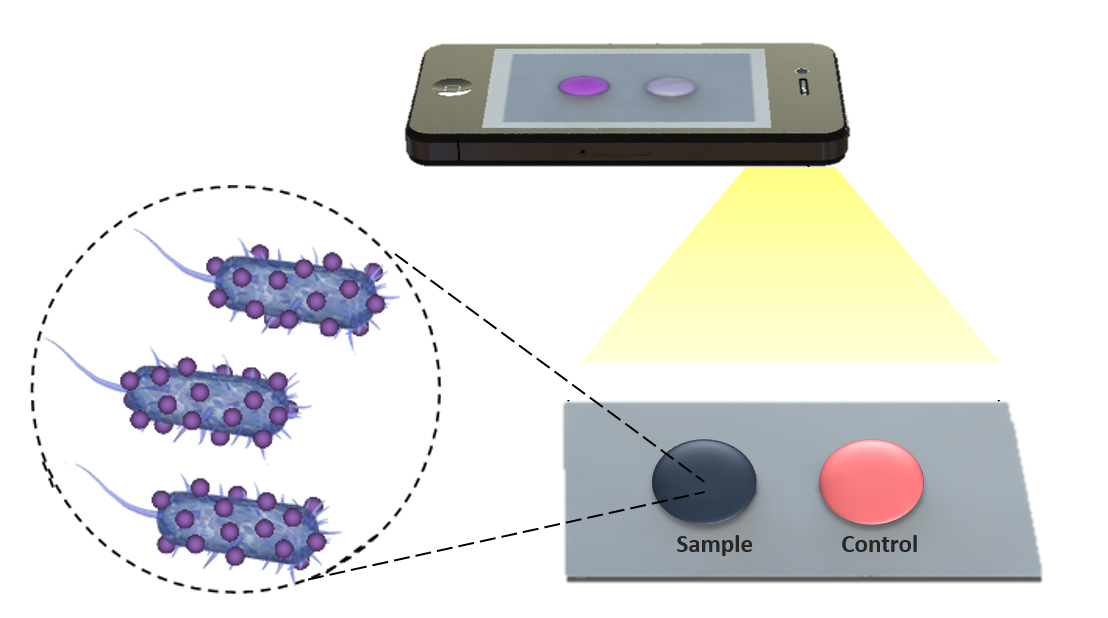
Cheap, flexible biosensor detects HIV, E-coli, Staph aureas
Florida Atlantic, Stanford, and Harvard researchers have developed a thin, lightweight, flexible “paper microchip” biosensing platform to detect and determine treatment for HIV, E-coli, Staphylococcus aureas and other bacteria. They have also created an app that could remotely detect bacteria and disease in the blood using mobile phone images. Current paper and flexible material-based platforms…
-
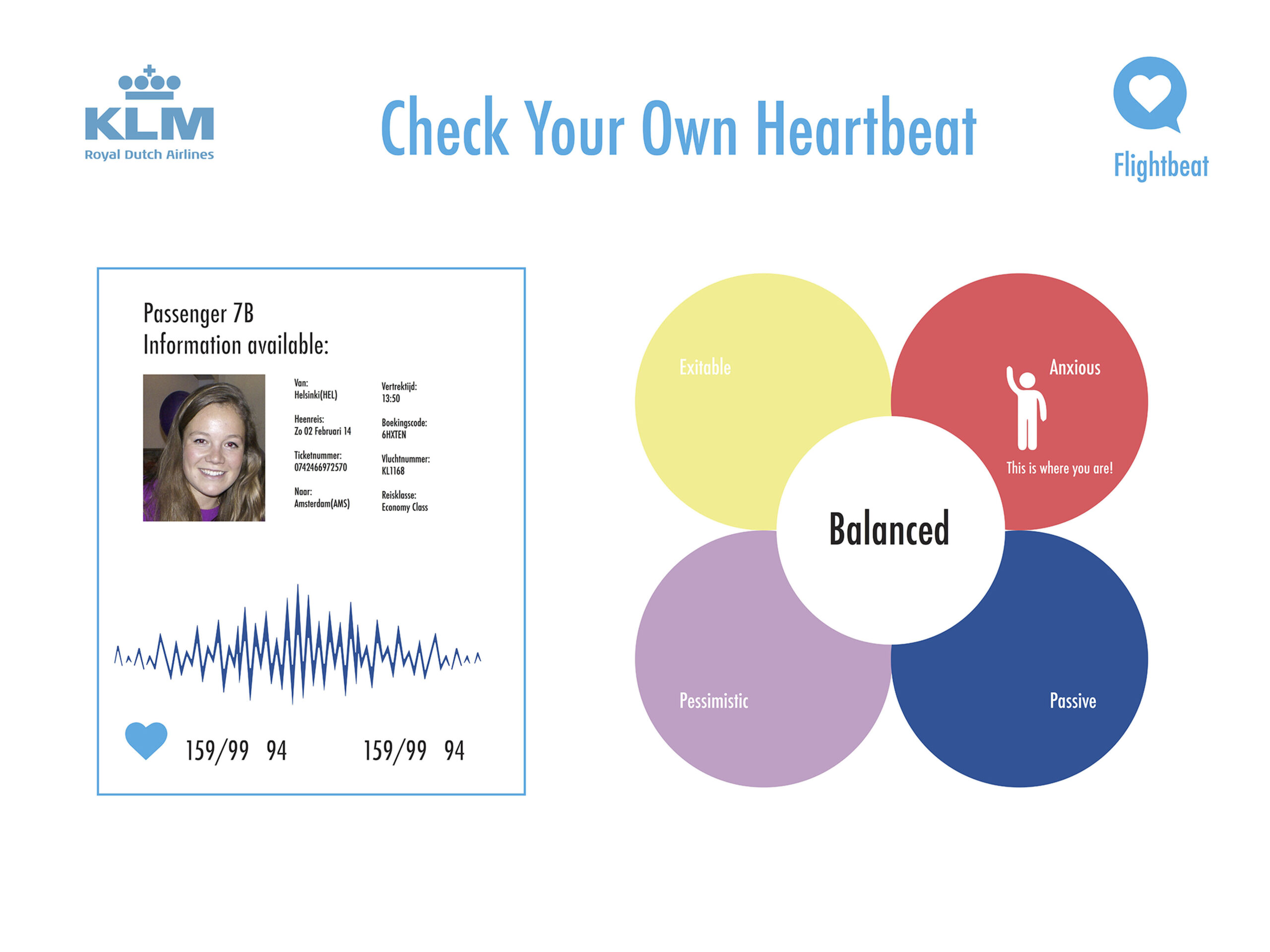
Airplane seat sensors monitor physical, emotional states
FlightBeat, designed by TU Delft students, uses airplane seat integrated heart rate sensors to monitor the physical and emotional state of passengers. Data is transmitted wirelessly to the crew, and presented on a color-coded seat map showing which passengers need attention. Health information can also be sent to physicians or family members on the ground. The goal…
-

Wearable detects asthma triggers
North Carolina State University‘s Veena Misra is developing a wearable that detects asthma triggers. The device monitors environmental factors, such as ozone, carbon monoxide and nitrogen dioxide levels, as well as vital signs including heart rate and hydration. Sensor data is transmitted wirelessly to a phone or physician’s office. The intention is to guide people away…
-
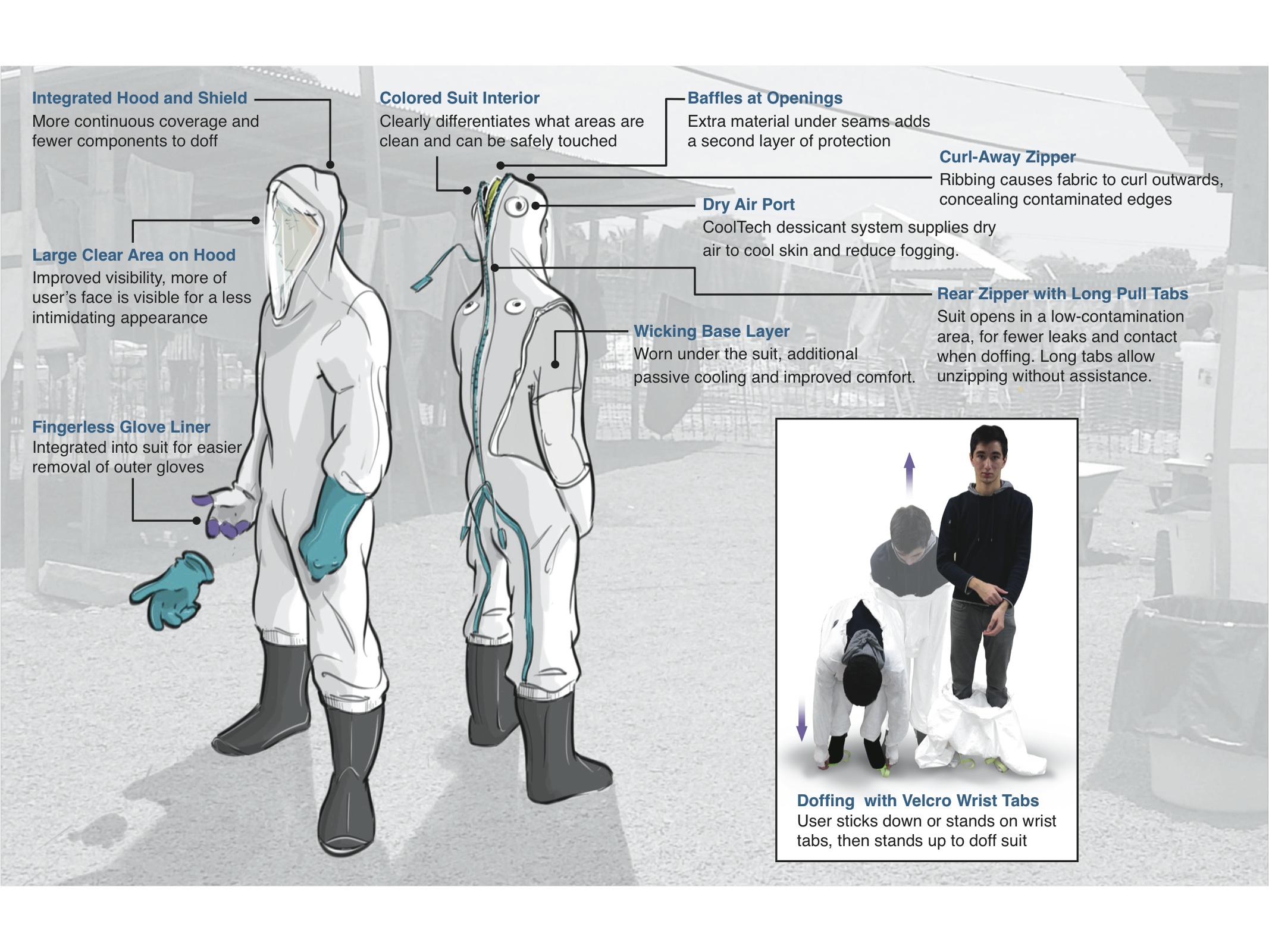
Suit, patch allow doctors to safely treat Ebola patients
At SXSW this week, USAID unveiled a biomedical suit and a wearable sensor patch to protect doctors while treating Ebola patients. The John’s Hopkins developed suit takes two minutes to put on. It has anti-fogging capabilities and will contain a cooling system, allowing doctors to wear it for longer periods. Past protective suits took 30 minutes to put on, were…
-

Paper test detects Ebola in 10 minutes
MIT‘s Hamad-Schifferli Group and Lee Gehrke have developed a paper strip test that can detect Ebola, Yellow Fever, and Dengue Fever in 10 minutes. The strips are color coded, using triangular silver nanoparticles, to distinguish among diseases. The test relies on lateral flow technology, used in pregnancy tests and for diagnosing strep throat and bacterial…
-
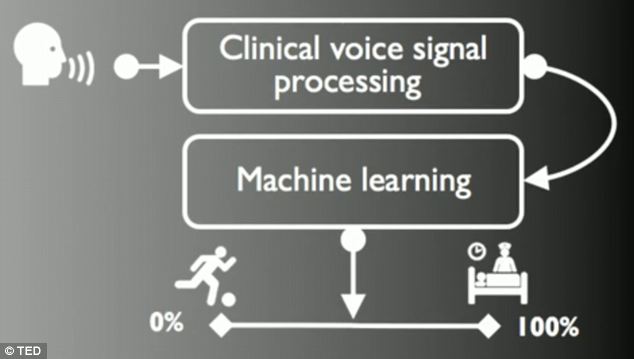
Smartphone tests detect Parkinson’s
In a recent study, MIT Media Lab‘s Max Little used machine learning tools to indicate early Parkinson’s Disease in a group of smartphone users. Phones were given to Parkinson’s patients and a healthy control group. The built in accelerometer enabled Little to distinguish between those with and with out the disease with 99% accuracy. The detection method relied…
-

Smartphone blood test detects HIV, Syphilis
Columbia bioengineering professor Samuel K. Sia has developed a cheap smartphone dongle that can detect three infectious disease markers from a finger prick of blood in 15 minutes. The device replicates mechanical, optical, and electronic functions of a lab based blood test. It performs an enzyme-linked immunosorbent assay without requiring stored energy, as power is drawn from…
-

App helps diagnose TBI in soldiers; can identify depression, PTSD
The US Army and AnthroTronix have developed an app that provides data to help diagnose and measure brain injuries in soldiers. The “DANA” includes 5, 20, and 45 minute neurocognitive tests and psychological survey questions. The data will help doctors diagnose traumatic brain injury and identify depression, post-traumatic stress, and other neurocognitive issues. The game-like test includes exercises…
-

Portable, lens free, on chip microscope for 3-D imaging
UCLA professor Aydogan Ozcan has developed a lens-free microscope for high throughput 3-D tissue imaging to detect cancer or other cell level abnormalities. Laser or light-emitting-diodes illuminate a tissue or blood sample on a slide inserted into the device. A sensor array on a microchip captures and records the pattern of shadows created by the sample. The…
-

Measuring body chemistry at home
Cue is a health tracker that measures inflammation, vitamin D levels, fertility, influenza, and testosterone. Its creators claim to bring tests that were previously only available in the lab into the home. The system sends customized alerts with suggestions on how to improve one’s health. . A droplet of saliva, blood, or a nasal swab…
-
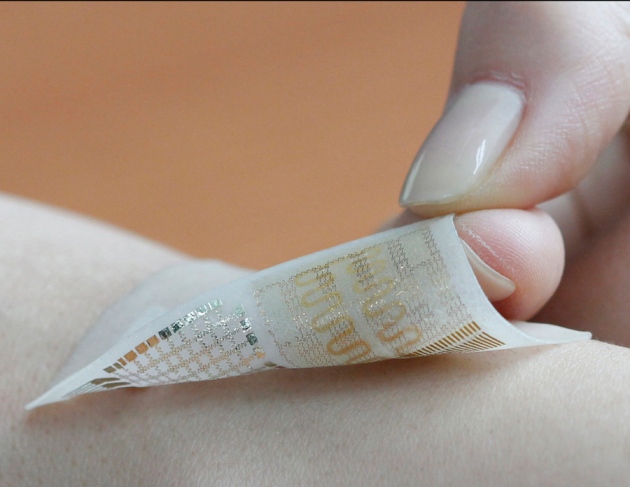
Patch monitors muscle activity, dispenses medicine
Kim Dae-Hyeong and colleagues at Seoul National University have created a dermal patch that measures and records muscle activity, dispenses medicine continuously, and stops drug delivery when appropriate. The study was published in Nature Nanotechnology today. The system is ideal for Parkinson’s patients, as tremors that accompany the movement disorder are not constant. The patch senses tremors early…